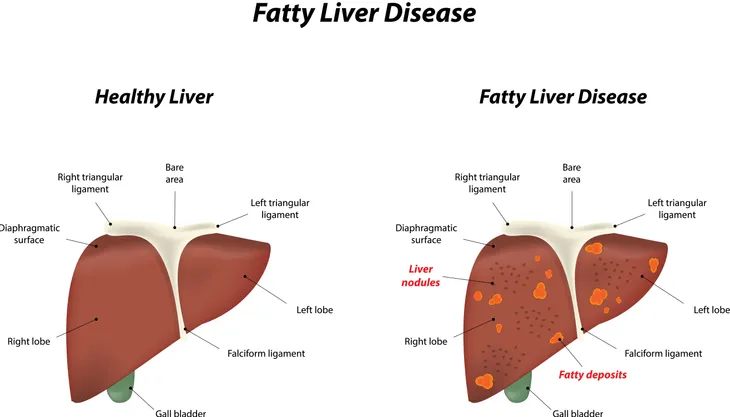
While excessive drinking can often lead to fatty deposits in the liver over time (and eventually to liver disease), there are other reasons a patient may end up with a fatty liver. Even if you don’t drink or are a moderate drinker, you can still be affected by non-alcoholic fatty liver disease (NAFLD).
While NAFLD generally isn’t a major concern on its own, if left unchecked, it can lead to other more serious health problems, with some forms of fatty liver disease causing major complications. Let’s look closer at 12 interesting facts about this condition…
What Is It?
This type of liver disease has nothing to do with excess drinking, it’s actually a result of a metabolic syndrome. WebMD describes metabolic syndrome as an umbrella term “marked by high blood pressure, high levels of bad cholesterol, [hormone that regulates the amount of glucose in the blood], and large amounts of belly fat.”
The National Institute of Diabetes and Digestive and Kidney Diseases describes NAFLD as a condition that occurs when there is a buildup of fat in the liver. This is not caused by heavy alcohol use and represents the body’s excess fat in the liver.
There Are Two Types
There are two separate types of NAFLD. The first is called simple fatty liver, and the second is nonalcoholic steatohepatitis (NASH). Even though they are both considered to be NAFLD, they are two separate conditions, notes NIH. So, what differentiates the two?
Simple fatty liver means “you have fat in your liver, but you may not have any inflammation in your liver or damage to your liver cells,” writes WebMD. This type of NAFLD isn’t serious, as it doesn’t tend to cause any problems with the liver or get any worse as time goes on.
The other type is referred to as NASH and is much more serious. “NASH means you have inflammation in your liver. You may also have damage to your liver cells,” explains the source. The inflammation and liver cell damage can cause other serious problems, such as fibrosis, which is scarring of the liver. It can also lead to cirrhosis, which is severe scarring that can lead to liver cancer, liver failure, and subsequent death. WebMD notes that nearly 20-percent of people with NAFLD have NASH.
There’s a Potentially Fatal Version
The Mayo Clinic explains that NAFLD is actually an umbrella term for a range of liver conditions that don’t have alcohol as a trigger. One form of the disease that might cause more alarm to patients and doctors is NASH, which is characterized by liver inflammation that can lead to scarring and permanent damage, notes the source.
This form of the disease, ironically, is similar to what might occur in a heavy drinker’s liver, explains the clinic. At its worst, this condition can lead to liver failure, which can cause death.
It’s Becoming Increasingly Common
The Mayo Clinic explains that the prevalence of NAFLD is increasing around the world, particularly in Western nations like the U.S. In fact, here at home it is the most common form of chronic liver disease, affecting up to 100-million people, according to the source.
It most commonly strikes people in their 40s and 50s, especially those who are at a higher risk of heart disease due to obesity or type 2 diabetes, it adds. However, it can occur in people of all age groups, notes the clinic.
Genetics Likely Play a Role
The University of California, San Diego explains that NAFLD is “shown to run in families,” and if you have a child diagnosed with the condition, you should also be tested during routine medical exams, even without symptoms.
The article quotes an expert that states, “As we suspected, NAFLD is not simply about weight, but rather is highly familial and likely genetic.” The source cites a study involving 44-children with or without NAFLD and 152-family members. “Whether or not the child had NAFLD was a major determinant of the amount of liver fat present in the other family members,” states the study. It found that 59-percent of siblings and 78-percent of parents related to children with NAFLD also had the disease.
Metabolic Syndrome Might Be a Link
A post on Science Direct explains there is growing evidence of a connection between NAFLD and metabolic syndrome, which is a “disease composed of different risk factors such as obesity, type 2 diabetes or dyslipidemia.” NAFLD is being recognized as the “liver manifestation” of the syndrome, it adds.
The prevalence of metabolic syndrome is rising as global obesity levels rise. A key characteristic linking NAFLD and metabolic syndrome is resistance to the hormone that regulate glucose in the blood, which can lead to high blood sugar and is associated with accumulation of fat in areas such as the liver. The resulting inflammation can further aggravate the resistance, creating a “vicious cycle,” explains the source.
There May Be No Symptoms
As we hinted at earlier, often you may not know you have NAFLD until it develops into something more serious. MedicineNet.com explains that early signs of the disease will show up in routine blood tests, or from ultrasonography when checking for other problems such as gallstones.
When the disease progresses, which is referred to as cirrhosis, the symptoms can be a lot more serious and may include the following: excessive bleeding due to the liver’s inability to produce blood-clotting proteins; jaundice (yellowing of the skin) from the liver’s inability to filter out bilirubin from the bloodstream; and fluid accumulation due to “portal hypertension” which causes fluid leakage from blood vessels, adds the source.
Symptoms That Can Exist
While non-alcoholic fatty liver disease often presents with no symptoms or warning signs, when they do occur, they often come in the form of an enlarged liver, fatigue, or pain in the upper right abdomen says the Mayo Clinic. You might also see elevated levels of liver enzymes, increased levels of the hormone that regulates glucose in the blood, and elevated triglyceride levels.
The Mayo Clinic also includes signs and symptoms of NASH which might present with symptoms such as “abdominal swelling, enlarged blood vessels beneath the skin’s surface, enlarged breasts in men, enlarged spleen, red palms,” and jaundice, which is yellowing of the skin and eyes.
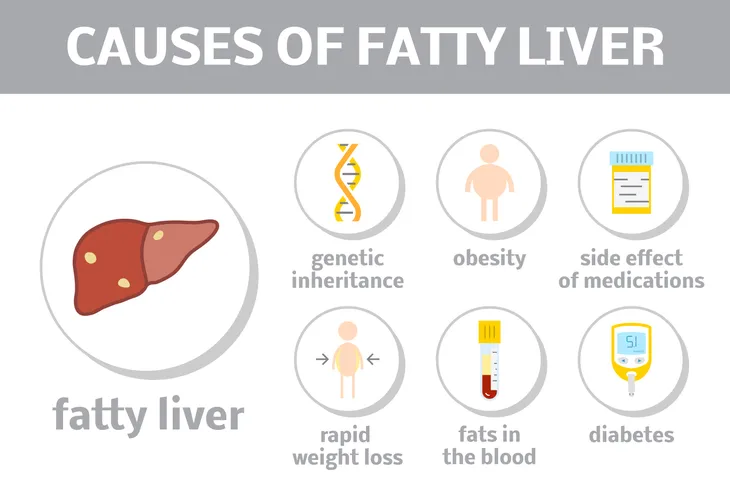
Most Common Causes
We already mentioned that NAFLD is not caused by alcohol and it’s due to a build-up of fat in the liver. Why does this happen? According to the Mayo Clinic, experts are still unclear why it happens to some people and not others. There is also little understanding of why there are two separate types of fatty liver (simple fatty liver and NASH). They still cannot find a definitive reason why one fatty liver becomes inflamed and leads to conditions such as cirrhosis and why another doesn’t.
What is known is that there are links to both NAFLD and NASH. The most common links are overweight or obesity, a resistance to the hormone that regulate glucose in the blood “in which your cells don’t take up sugar in response to the hormone,” and high blood sugar (hyperglycemia) which are found in people with prediabetes or type 2 diabetes. It’s also linked to high levels of fat in the blood, particularly triglycerides, says the Mayo Clinic.
Complications of Fatty Liver Disease
The most common complication of fatty liver disease is cirrhosis which is late-stage scarring of the liver. “Cirrhosis occurs in response to liver injury, such as the inflammation in nonalcoholic steatohepatitis,” writes the Mayo Clinic. “As the liver tries to halt inflammation, it produces areas of scarring (fibrosis). With continued inflammation, fibrosis spreads to take up more and more liver tissue,” adds the source.
Cirrhosis is a serious condition that can progress and lead to fluid build-up in the abdomen, swelling of the veins in the esophagus (which can later rupture and bleed), liver cancer, end-stage liver failure, confusion, drowsiness, and slurred speech. The Mayo Clinic notes that 20-percent of people with NASH will develop cirrhosis.
How to Prevent a Fatty Liver
In order to reduce your risk of developing fatty liver disease, you can make healthier choices when it comes to diet, exercise, and overall lifestyle. The Mayo Clinic suggests eating more plant-based foods such as fruits, vegetables, whole grains, and healthy fats. At the same time, you should be cutting back on carbs, particularly refined carbs. While researchers report that only 16-percent of people with NAFLD have liver fat from diet, Healthline points to some research that has shown that a diet low in refined carbs can reverse NAFLD.
You should work toward maintaining a healthy weight. If you are obese or overweight, you should be actively trying to lose the weight through a healthy diet and exercise. Healthline notes that weight loss has proven to be effective at promoting liver fat loss in adults with NAFLD.
Lastly, we should all be exercising frequently throughout the week. “Studies have shown that engaging in endurance exercise or resistance training several times a week can significantly reduce the amount of fat stored in liver cells, regardless of whether weight loss occurs,” writes Healthline.
Medical Treatments are Lacking
The American Liver Foundation notes there are currently no medically approved treatments in the U.S. for NAFLD. It instead says lifestyle changes are in order. “Eating a healthy diet and exercising regularly may help prevent liver damage from starting or reverse it in the early stages,” notes the source.
The source also reminds you to visit a liver specialist regularly to monitor the progression of the disease and to lower your intake of cholesterol and saturated fats that can raise levels of triglycerides (which store fat). Oh, and it should go without saying — but try to avoid alcohol too, even though it’s not the root cause of your problem.