Waking up flushed and covered in perspiration can occur after a particularly disturbing nightmare, but several external causes can also result in excess sweating throughout the night. For instance, your bedroom may simply be too hot or your body may be trying to fight off an infection. However, chronic night sweats often indicate an underlying health condition (i.e., hypoglycemia or perimenopause).
The eight most common causes of night sweating are…
1. Overheating
If you like to sleep in sweatpants (or in fuzzy pajamas like me) night sweats can occur during the night if your body overheats. This is typically and innocently due to a combination of high temperature and thick pajamas.
Sweating due to overheating will usually cause flushing and mild perspiration. Alternately, characteristic night sweats are often far more extreme, according to WebMD, causing numerous hot flashes during the night that have you waking up wet with perspiration that saturates your bedclothes, the sheets, and the mattress.
2. Certain Prescription Drugs
There are several prescription drugs that state night sweats among their side effects. For instance, researchers at the Perelman School of Medicine, in the Department of Psychiatry at the University of Pennsylvania, report that prescribed antidepressant medications have been linked to antidepressant-induced excessive sweating (ADIES), a form of severe night sweats, in roughly 14-percent of patients prescribed these medicines.
In addition to prescription drugs, many doctors credit common over-the-counter medicines, such as acetaminophen and aspirin, for causing night sweats. This is most prevalent when these medications are taken to break a fever.
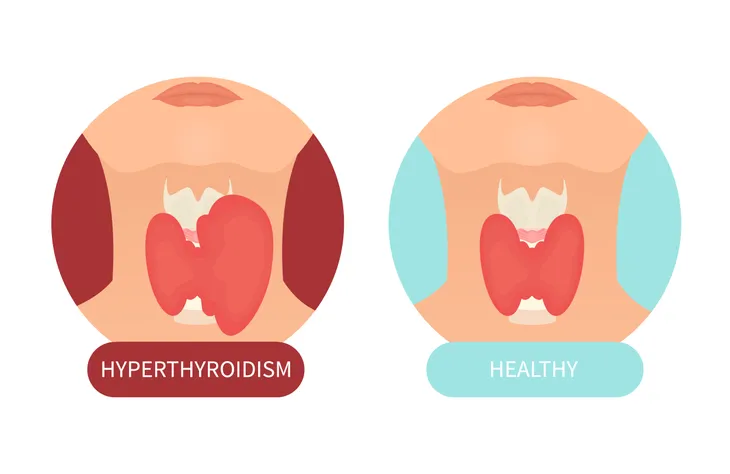
3. Hyperthyroidism
Hyperthyroidism, or an overactive thyroid gland that produces excessive levels of thyroid hormone (thyroxine), will understandably result in chronic night sweats. One of the prime symptoms of an overactive thyroid (and other hormonal disorders such as carcinoid syndrome) is heat intolerance and excessive perspiration.
A collaborative research study conducted by doctors at Florida’s Jacksonville Naval Hospital and Maryland’s National Naval Medical Center in Bethesda concluded the characteristics of increased heart rate, health palpitations, anxiety, restless legs, weight loss, and irregular menstrual cycles associated with hyperthyroidism can understandably result in night sweats while sleeping.
4. Certain Types of Cancer
Night sweats can also be a secondary symptom that indicates the existence of certain undiagnosed cancers, particularly Hodgkin’s lymphoma (or Hodgkin’s disease), which is a cancer of the white blood cells (specifically the type referred to as lymphocytes).
A research study from physicians at the College of Medicine, at the University of Oklahoma Health Sciences Center, listed night sweats among the “B symptoms” of lymphoma. Other B symptoms of lymphoma include itchy skin, fever, and unexplained weight loss.
5. Hypoglycemia
The American Diabetes Association considers night sweats a very common symptom of hypoglycemia, or bouts of low blood sugar (below 50 mg/dL).
Many patients with diabetes that take prescription insulin or oral diabetes medications may also experience nighttime hypoglycemia, or episodes of plummeting blood sugar (glucose) while sleeping. During sleep, blood glucose is difficult to maintain, as the pancreas doesn’t secrete the hormone that regulates glucose in the blood, and night sweats can result.
6. Infections and Viruses
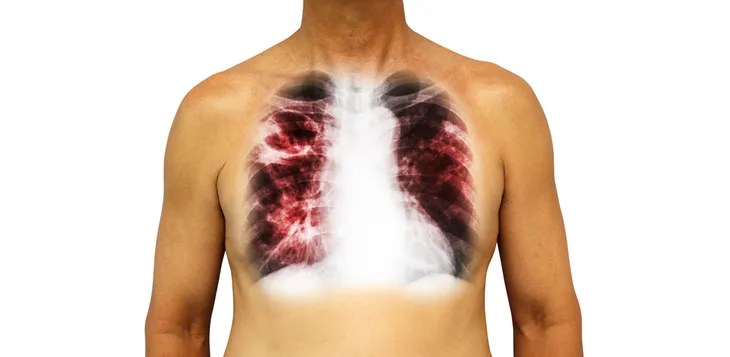
Several types of infections—most notably, tuberculosis (TB), human immunodeficiency virus (HIV), endocarditis (bacterial infection of the heart valves), abscesses, and osteomyelitis (bone infection)—will cause fever and night sweats.
According to a research paper entitled “Diagnosing Night Sweats” and published by the journal, American Family Physician, infections, such as TB and HIV, which present with low-grade fever and chills, weight loss, and cough, can also cause a fever at night along with night sweats as later complications of the diseases.
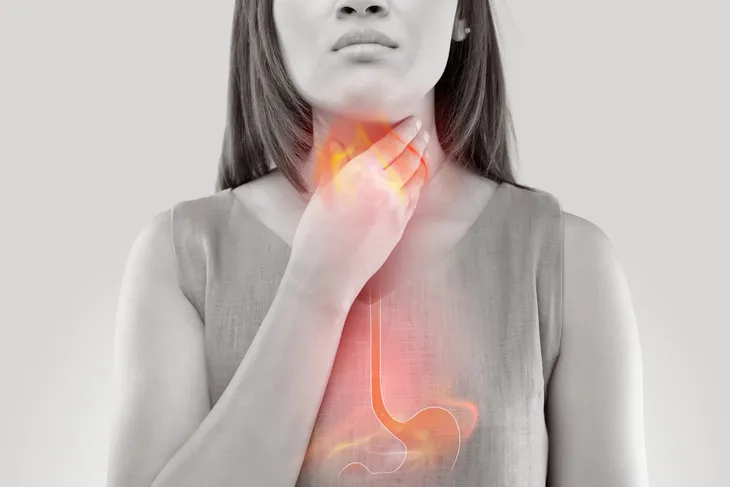
7. Gastroesophageal Reflux Disease
According to a research study from Harvard Medical School, gastroesophageal reflux disease (GERD) is often linked to night sweats, along with symptoms of chronic cough with bloody sputum (hemoptysis), wheezing or shortness of breath, fatigue, and chest pain.
You should bring chronic night sweats to your doctor’s attention and keep a thorough journal whenever you wake up during the night to record temperature variations, flushing, and perspiration levels. The research suggests that once GERD is diagnosed and treated, complete relief from night sweats usually occurs quickly.
8. Menopause
Additional research from epidemiologists at Harvard School of Public Health and published in the journal JAMA Internal Medicine claims that the hormonal fluctuations that occur with menopause (marking the end of women’s childbearing years) will often trigger vasomotor symptoms, such as hot flashes, chills, flushing, excessive perspiration, and night sweats during sleep.
Harvard statistics indicate that approximately 80-percent of women going through menopause will experience night sweats so severe that they will chronically disturb sleep. While estrogen-based hormone replacement therapy (HRT) is one option for relieving hot flashes and night sweats, hormone therapy has been linked to increased risks for breast cancer, blood clots, and stroke. So be sure to explore all of your options with the help of your doctor.