Dementia refers to a group of symptoms that affect memory, thinking, and social skills severely enough to interfere with daily functioning. It is not a specific disease, but a group of symptoms caused by various diseases and conditions. No one test can determine if an individual has dementia.
Dementia does not have a cure, and no treatment can totally halt its progression. Alzheimer’s is the most common type of dementia, accounting for 60 to 80-percent of cases. Vascular dementia, previously known as post-stroke dementia, is the second most common type of dementia, accounting for 10-percent of cases.
The 10 risk factors for dementia are…
Advancing Age
The primary risk factor for developing dementia is advancing age. The risk of dementia greatly increases after the age of 65. The Alzheimer’s Association reports the likelihood of developing Alzheimer’s dementia doubles every 5-years after the age of 65. The National Institute of Neurological Disorders and Stroke estimates as many as 5-million Americans age 65 and older may have Alzheimer’s dementia. As a result, the number of Americans living with dementia could double in the next 40-years as the number of Americans age 65 and older increases from 40-million today to greater than 88-million in the year 2050.
After the age of 85, the risk of developing Alzheimer’s dementia reaches nearly 50-percent. Despite these staggering numbers, the commonly held belief that dementia is a normal part of aging is erroneous. Dementia is not a normal part of aging, and some individuals may experience dementia at a relatively young age.
Genetic Factors
Individuals with a first-degree relative (parent, sibling, or child) diagnosed with Alzheimer’s dementia are more likely to develop the condition. The risk is further increased if more than one family member has the condition. Despite this fact, many individuals with a family history of dementia do not develop the disorder, and many individuals without a family history of dementia go on to develop the disorder.
Genetic testing is available for Alzheimer’s dementia. The gene with the strongest correlation to the development of dementia is apolipoprotein E4, or ApoE4. Individuals who inherit one copy of the ApoE4 gene are at a twofold to fourfold increased risk for developing Alzheimer’s dementia. Individuals who inherit two copies of the gene have a tenfold higher risk, but are not certain to develop dementia. Inheritance of this gene may also be implicated in the onset of dementia at a relatively young age. Routine genetic testing for dementia is not recommended and is usually done as part of research studies.
Female Gender
Gender seems to play a role in the development of dementia. Several clinical studies have suggested that women are at higher risk for dementia than men. A Dutch study showed that after 90-years of age the incidence of dementia, particularly Alzheimer’s dementia, is higher for women than for men. According to the United States census, the 90-plus age group is the fastest growing segment of the population. Women comprise three-quarters of the 90-plus age group population. The findings noted may be explained by a protective effect of estrogen in premenopausal women.
A study published in Annals of Neurology found that women with one copy of the ApoE4 gene were at higher risk for the development of Alzheimer’s dementia than were men. Alzheimer’s dementia also seems to affect women differently than men in terms of behavior. Women with Alzheimer’s dementia tend to become more reclusive and emotionally unstable, while men tend to develop more aggression as the condition progresses.
Smoking
Researchers in Finland found individuals who were heavy smokers, defined as smoking greater than 2-packs of cigarettes daily, in their midlife years (age 50 to 60), were more than doubling their risk of developing dementia. Smoking is already a well-established risk factor for diseases such as heart disease, hypertension, cancer, and strokes. In the Finnish study, approximately 25-percent of participants were diagnosed with dementia an average of 23-years after the conclusion of the study.
In the same Finnish study, former smokers or individuals who smoked less than ½-pack of cigarettes per day did not appear to have an increased risk of developing dementia. Another study from Australia concluded that elderly smokers have increased risks of dementia and cognitive decline. Smoking may increase the risk of vascular dementia by its hand in the promotion of strokes. It is felt that oxidative stress and inflammation caused by smoking has a causative role in the development of Alzheimer’s disease.
Excessive Alcohol Consumption
Excessive alcohol consumption has been proposed as a possible risk factor for cognitive impairment and dementia. A Chinese study concluded excessive alcohol consumption was related to a higher risk of dementia. In the same Chinese study, light to moderate alcohol consumption was associated with a significantly lower risk of dementia compared with non-drinkers. In the literature, this is described as a U-shaped relationship.
A study published in the British Medical Journal also found a U-shaped relationship between alcohol consumption and the risk of developing dementia. In other words, light to moderate alcohol consumption may have a protective effect against the development of dementia compared with non-drinking, while heavy alcohol consumption seems to increase the risk of dementia. The effects observed seem to be independent of the type of alcohol. In the same study, the risk of dementia increased with increasing frequency of alcohol consumption among those carrying the ApoE4 gene, which is the gene with the strongest correlation to the development of dementia.
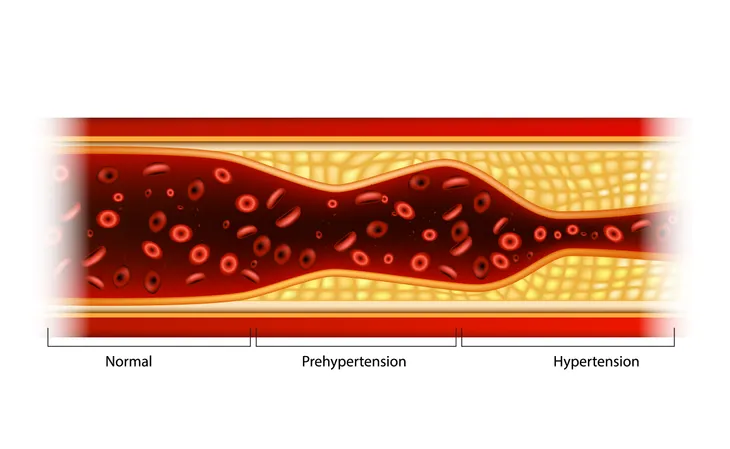
Hypertension
Hypertension, also known as high blood pressure, is a very powerful risk factor for dementia, including vascular and Alzheimer’s dementia. Long-term hypertension carries the risk of damaging small arteries in the brain, which may impede blood flow and result in atrophy of brain tissue. These mechanisms may lead to cognitive impairment and dementia. In individuals younger than 60-years, hypertension is defined as a blood pressure greater than 140/90 mm Hg. In individuals older than 60-years, it is defined as a blood pressure greater than 150/90 mm Hg. The components of blood pressure are the systolic blood pressure (the number on top) and diastolic blood pressure (the number on the bottom).
A long-term (20 years) study published in Hypertension concluded a high diastolic blood pressure at age 50 correlated with poorer cognitive performance at age 70. In the same study, the risk of dementia was more than doubled if systolic blood pressure was in or above the range of 140-160 mm Hg. (Learn more Possible Complications of Hypertension).
Diabetes
Type 2 diabetes, formerly known as adult-onset diabetes, has long been a risk factor for strokes. Strokes are the underlying factor in the development of vascular dementia. A Dutch study published in Neurology concluded individuals suffering from diabetes were at increased risk for dementia, including Alzheimer’s dementia. The association was strongest in those individuals receiving the hormone that regulates glucose in the blood as part of their treatment for diabetes.
Examination of the brains of individuals suffering from diabetes revealed over expression of a protein named beta-amyloid, which is found in the plaques and tangles of Alzheimer’s dementia. Excessive beta-amyloid is felt to cause oxidative stress that leads to cellular brain damage. A study published in the New England Journal of Medicine established an increased risk of dementia in individuals with elevated blood sugars not in the diabetic range. Those with elevated blood sugars not in the diabetic range would be termed to have impaired fasting glucose or impaired glucose tolerance.
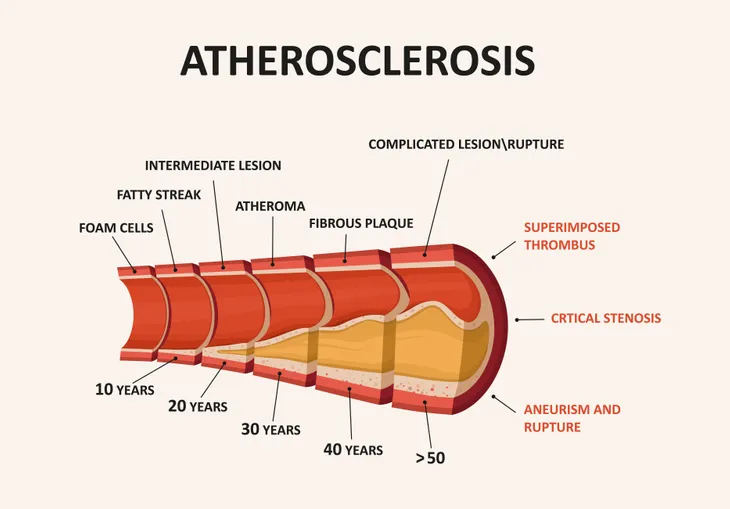
Atherosclerosis
Atherosclerosis represents the deposition of fat, cholesterol, and other substances into the inner lining of an artery. It has long been an established risk factor for heart disease. It can reduce blood flow to the brain and lead to strokes, which can lead to vascular dementia. Excessive levels of low-density lipoprotein (LDL), also called “bad” cholesterol, often lead to atherosclerosis.
A Dutch study published in the Annals of Neurology concluded atherosclerosis, predominantly carotid artery atherosclerosis, was associated with an increased risk of dementia. The carotid arteries are found in the neck along either side of the windpipe. A study done at Johns Hopkins in Baltimore, MD concluded intracranial atherosclerosis, but not in the heart or aorta, significantly increased the risk of dementia. Intracranial atherosclerosis can be found within the skull in the arteries of the brain. It establishes intracranial atherosclerosis as an independent and important risk factor for dementia.
Obesity
Obesity is defined as a body mass index (BMI) greater than 30 kg/m2. The BMI is an indirect measure of body fat based on weight (in kilograms) and height (in meters). The measure has long been used to estimate the risk of developing chronic diseases such as hypertension, diabetes, and heart disease. It is thought 50-percent of adults have central obesity. Researchers now feel there may be a connection between increased BMI and the development of dementia.
A study from Harvard Medical School concluded that increased BMI is independently associated with an increased risk of dementia. Another study from the Karolinska Institutet in Sweden found midlife obesity was associated with an increased risk of dementia, including Alzheimer’s dementia, later in life. Lastly, a study published in Neurology found central obesity in midlife correlated with an increased risk of dementia independent of diabetes and other cardiovascular diseases.
Elevated Homocysteine Blood Levels
Homocysteine is an amino acid. Amino acids are the building blocks of proteins. Elevated homocysteine blood levels have been associated with heart disease, stroke, and abnormal blood clot formation. Abnormal blood clot formation may lead to life threatening conditions such as deep vein thrombosis (DVT) and pulmonary embolism (PE). A homocysteine blood level above 15-micromoles/liter is considered high. Optimal homocysteine blood levels are below 10 to 12-micromoles/liter. It is thought the condition may be due to dietary deficiencies in vitamin B6, vitamin B12, and folic acid.
Researchers are concerned that elevated homocysteine blood levels may play a role in the development of dementia. Researchers at Boston University published a study in the New England Journal of Medicine that found elevated levels of homocysteine in the blood nearly doubled the risk of developing Alzheimer’s disease. A recent study published in the Proceedings of the National Academy of Sciences revealed B-vitamin supplementation halted atrophy, or wasting, in areas of the brain associated with Alzheimer’s dementia and slowed cognitive decline.